Connect With Us
Blog
Blog
Improving Poor Circulation
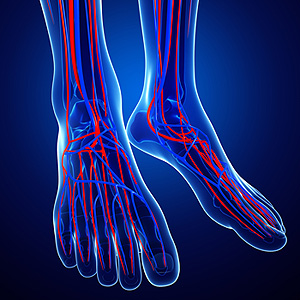 Poor circulation, or inadequate blood flow to the lower extremities, is common in people with underlying health conditions, such as peripheral artery disease, and for the elderly. Common causes of poor circulation to the lower limbs include obesity, varicose veins, and blood clots. Fortunately, there are things that you can do to improve circulation to your legs and feet. Walking is a low impact exercise that you can do daily to increase blood flow to the legs. If you are a smoker, quitting can reduce damage to your blood vessels, thereby improving circulation. Finally, eating a balanced diet and staying hydrated can improve overall health, including the health of your circulatory system. If you have poor circulation to your legs and feet, it is suggested that you visit a podiatrist, who can help you treat, manage and prevent complications associated with poor circulation.
Poor circulation, or inadequate blood flow to the lower extremities, is common in people with underlying health conditions, such as peripheral artery disease, and for the elderly. Common causes of poor circulation to the lower limbs include obesity, varicose veins, and blood clots. Fortunately, there are things that you can do to improve circulation to your legs and feet. Walking is a low impact exercise that you can do daily to increase blood flow to the legs. If you are a smoker, quitting can reduce damage to your blood vessels, thereby improving circulation. Finally, eating a balanced diet and staying hydrated can improve overall health, including the health of your circulatory system. If you have poor circulation to your legs and feet, it is suggested that you visit a podiatrist, who can help you treat, manage and prevent complications associated with poor circulation.
Poor circulation is a serious condition and needs immediate medical attention. If you have any concerns with poor circulation in your feet contact Julie Jurd-Sadler, DPM of Progressive Podiatry. Our doctor will treat your foot and ankle needs.
Poor Circulation in the Feet
Poor blood circulation in the feet and legs is can be caused by peripheral artery disease (PAD), which is the result of a buildup of plaque in the arteries.
Plaque buildup or atherosclerosis results from excess calcium and cholesterol in the bloodstream. This can restrict the amount of blood which can flow through the arteries. Poor blood circulation in the feet and legs are sometimes caused by inflammation in the blood vessels, known as vasculitis.
Causes
Lack of oxygen and oxygen from poor blood circulation restricts muscle growth and development. It can also cause:
- Muscle pain, stiffness, or weakness
- Numbness or cramping in the legs
- Skin discoloration
- Slower nail & hair growth
- Erectile dysfunction
Those who have diabetes or smoke are at greatest risk for poor circulation, as are those who are over 50. If you have poor circulation in the feet and legs it may be caused by PAD and is important to make changes to your lifestyle in order to reduce risk of getting a heart attack or stroke. Exercise and maintaining a healthy lifestyle will dramatically improve conditions.
As always, see a podiatrist as he or she will assist in finding a regimen that suits you. A podiatrist can also prescribe you any needed medication.
If you have any questions please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
A Common Reason Blisters Develop on the Feet
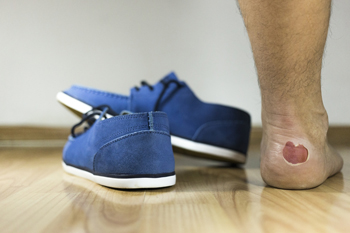 The definition of a blister is a small pocket that is filled with fluid. This can develop as a result of consistent friction that can come from wearing shoes and socks that do not fit correctly. It is the body’s natural healing response to skin that has become damaged. When new skin has formed under the blister, it will gradually drain, and is no longer needed. It may be helpful to protect the blister with a protective covering while daily activities are being completed. It is beneficial to remove the covering or bandage while sleeping as this may help to accelerate the healing process. Blisters may be prevented by wearing shoes and socks that fit correctly, and this can be accomplished when they are purchased in the afternoon, when the feet are at their largest. If you would like additional information on how to treat and prevent blisters from developing on the feet, please speak with a podiatrist.
The definition of a blister is a small pocket that is filled with fluid. This can develop as a result of consistent friction that can come from wearing shoes and socks that do not fit correctly. It is the body’s natural healing response to skin that has become damaged. When new skin has formed under the blister, it will gradually drain, and is no longer needed. It may be helpful to protect the blister with a protective covering while daily activities are being completed. It is beneficial to remove the covering or bandage while sleeping as this may help to accelerate the healing process. Blisters may be prevented by wearing shoes and socks that fit correctly, and this can be accomplished when they are purchased in the afternoon, when the feet are at their largest. If you would like additional information on how to treat and prevent blisters from developing on the feet, please speak with a podiatrist.
Blisters are prone to making everyday activities extremely uncomfortable. If your feet are hurting, contact Julie Jurd-Sadler, DPM of Progressive Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Foot Blisters
Foot blisters develop as a result of constantly wearing tight or ill-fitting footwear. This happens due to the constant rubbing from the shoe, which can often lead to pain.
What Are Foot Blisters?
A foot blister is a small fluid-filled pocket that forms on the upper-most layer of the skin. Blisters are filled with clear fluid and can lead to blood drainage or pus if the area becomes infected.
How Do Blisters Form?
Blisters on the feet are often the result of constant friction of skin and material, usually by shoe rubbing. Walking in sandals, boots, or shoes that don’t fit properly for long periods of time can result in a blister. Having consistent foot moisture and humidity can easily lead to blister formation.
Prevention & Treatment
It is important to properly care for the affected area in order to prevent infection and ease the pain. Do not lance the blister and use a Band-Aid to provide pain relief. Also, be sure to keep your feet dry and wear proper fitting shoes. If you see blood or pus in a blister, seek assistance from a podiatrist.
If you have any questions, please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Heel Pain Can Be Treated!
The Importance of Practicing Foot Care for Diabetic Patients
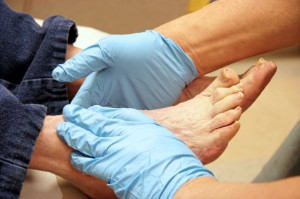 Patients who are diabetic may be fearful of losing a toe or foot due to their condition. Foot complications can occur as a result of elevated blood sugar levels and can cause the feet to feel numb or minimal sensation. This may lead to the inability to feel existing cuts or bruises on the feet, and diabetic ulcers may develop. It is beneficial to implement a daily foot care routine. This can consist of washing the feet every day, properly trimming the toenails, and maintaining steady blood circulation. It is helpful to smooth corns and calluses by utilizing a pumice stone, and this can aid in preventing foot infections from developing. If you have diabetes, it is strongly suggested that you are under the care of a podiatrist who can guide you toward proper management techniques.
Patients who are diabetic may be fearful of losing a toe or foot due to their condition. Foot complications can occur as a result of elevated blood sugar levels and can cause the feet to feel numb or minimal sensation. This may lead to the inability to feel existing cuts or bruises on the feet, and diabetic ulcers may develop. It is beneficial to implement a daily foot care routine. This can consist of washing the feet every day, properly trimming the toenails, and maintaining steady blood circulation. It is helpful to smooth corns and calluses by utilizing a pumice stone, and this can aid in preventing foot infections from developing. If you have diabetes, it is strongly suggested that you are under the care of a podiatrist who can guide you toward proper management techniques.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact Julie Jurd-Sadler, DPM from Progressive Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
- Routinely inspect your feet for bruises or sores.
- Wear socks that fit your feet comfortably.
- Wear comfortable shoes that provide adequate support.
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Possible Treatment of a Broken Foot
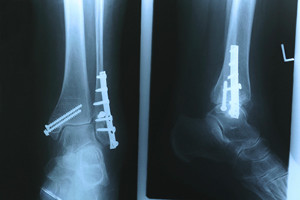 A common reason a broken foot may occur can be from falling off of a ladder, or it may become injured from participating in sporting events. The bones that are located between the toes and the ankle are referred to as the metatarsals. They can be prone to stress fractures, which typically happen from overuse. The average healing time for a broken foot is generally six to twelve weeks. Many daily activities are able to be completed as the healing process occurs when a walking boot or cast is worn. For more severe fractures, it may take longer if surgery is required. If you have pain in your feet as a result of either a fall or something else, it is advised that you consult with a podiatrist.
A common reason a broken foot may occur can be from falling off of a ladder, or it may become injured from participating in sporting events. The bones that are located between the toes and the ankle are referred to as the metatarsals. They can be prone to stress fractures, which typically happen from overuse. The average healing time for a broken foot is generally six to twelve weeks. Many daily activities are able to be completed as the healing process occurs when a walking boot or cast is worn. For more severe fractures, it may take longer if surgery is required. If you have pain in your feet as a result of either a fall or something else, it is advised that you consult with a podiatrist.
A broken foot requires immediate medical attention and treatment. If you need your feet checked, contact Julie Jurd-Sadler, DPM from Progressive Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Broken Foot Causes, Symptoms, and Treatment
A broken foot is caused by one of the bones in the foot typically breaking when bended, crushed, or stretched beyond its natural capabilities. Usually the location of the fracture indicates how the break occurred, whether it was through an object, fall, or any other type of injury.
Common Symptoms of Broken Feet:
- Bruising
- Pain
- Redness
- Swelling
- Blue in color
- Numbness
- Cold
- Misshapen
- Cuts
- Deformities
Those that suspect they have a broken foot shoot seek urgent medical attention where a medical professional could diagnose the severity.
Treatment for broken bones varies depending on the cause, severity and location. Some will require the use of splints, casts or crutches while others could even involve surgery to repair the broken bones. Personal care includes the use of ice and keeping the foot stabilized and elevated.
If you have any questions please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Possible Causes of Bunions
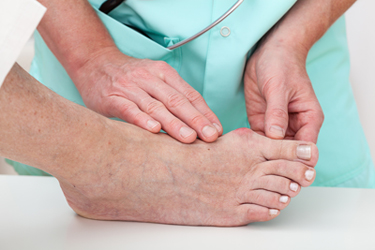 A bump that extends on the side of the big toe may indicate a bunion. It is considered to be a deformity, and a common cause can be from wearing shoes that do not have adequate room for the toes to move freely in. Additionally, genetics can play a significant role in developing a bunion. Mild relief may be found when larger shoes are purchased, and it may help to wear a protective covering over the top of the bunion. In severe cases, orthotics can be prescribed, and therapy techniques may be suggested. If you notice a bony protrusion on the side of the big toe, it may be a bunion, and it is strongly suggested that you seek treatment from a podiatrist.
A bump that extends on the side of the big toe may indicate a bunion. It is considered to be a deformity, and a common cause can be from wearing shoes that do not have adequate room for the toes to move freely in. Additionally, genetics can play a significant role in developing a bunion. Mild relief may be found when larger shoes are purchased, and it may help to wear a protective covering over the top of the bunion. In severe cases, orthotics can be prescribed, and therapy techniques may be suggested. If you notice a bony protrusion on the side of the big toe, it may be a bunion, and it is strongly suggested that you seek treatment from a podiatrist.
If you are suffering from bunions, contact Julie Jurd-Sadler, DPM of Progressive Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
A bunion is formed of swollen tissue or an enlargement of boney growth, usually located at the base joint of the toe that connects to the foot. The swelling occurs due to the bones in the big toe shifting inward, which impacts the other toes of the foot. This causes the area around the base of the big toe to become inflamed and painful.
Why Do Bunions Form?
Genetics – Susceptibility to bunions are often hereditary
Stress on the feet – Poorly fitted and uncomfortable footwear that places stress on feet, such as heels, can worsen existing bunions
How Are Bunions Diagnosed?
Doctors often perform two tests – blood tests and x-rays – when trying to diagnose bunions, especially in the early stages of development. Blood tests help determine if the foot pain is being caused by something else, such as arthritis, while x-rays provide a clear picture of your bone structure to your doctor.
How Are Bunions Treated?
- Refrain from wearing heels or similar shoes that cause discomfort
- Select wider shoes that can provide more comfort and reduce pain
- Anti-inflammatory and pain management drugs
- Orthotics or foot inserts
- Surgery
If you have any questions, please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Two Types of Corns
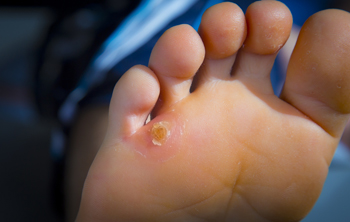 A corn is an area of skin that develops in a circular shape and is often found on the bottom of the foot or between the toes. It typically forms as a result of excess friction that can come from wearing shoes that do not fit correctly. Additionally, a corn can develop on the inside of the heel from existing medical conditions that can include flat feet. Hard corns can develop on top of the toes or on the sole of the foot. A corn that is found between the toes is referred to as a soft corn and can cause pain and discomfort. Relief may be found when the feet are washed and dried thoroughly, and it may also help to file the corn with a pumice stone. If you have a corn that is hindering daily activities, it is strongly advised that you consult with a podiatrist who can treat this condition properly.
A corn is an area of skin that develops in a circular shape and is often found on the bottom of the foot or between the toes. It typically forms as a result of excess friction that can come from wearing shoes that do not fit correctly. Additionally, a corn can develop on the inside of the heel from existing medical conditions that can include flat feet. Hard corns can develop on top of the toes or on the sole of the foot. A corn that is found between the toes is referred to as a soft corn and can cause pain and discomfort. Relief may be found when the feet are washed and dried thoroughly, and it may also help to file the corn with a pumice stone. If you have a corn that is hindering daily activities, it is strongly advised that you consult with a podiatrist who can treat this condition properly.
If you have any concerns regarding your feet and ankles, contact Julie Jurd-Sadler, DPM of Progressive Podiatry. Our doctor will treat your foot and ankle needs.
Corns: What Are They? and How Do You Get Rid of Them?
Corns can be described as areas of the skin that have thickened to the point of becoming painful or irritating. They are often layers and layers of the skin that have become dry and rough, and are normally smaller than calluses.
Ways to Prevent Corns
There are many ways to get rid of painful corns such as wearing:
- Well-fitting socks
- Comfortable shoes that are not tight around your foot
- Shoes that offer support
Treating Corns
Treatment of corns involves removing the dead skin that has built up in the specific area of the foot. Consult with Our doctor to determine the best treatment option for your case of corns.
If you have any questions please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Possible Treatments for an Achilles Tendon Injury
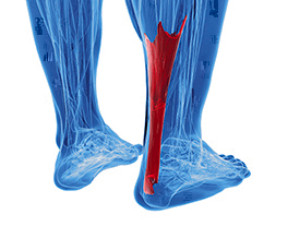 The Achilles tendon connects the heel to the calf muscles. It is located in the back of the leg, near the foot, and is responsible for the ability to point and flex the foot. An injury can cause the Achilles tendon to become ruptured or injured, and this generally causes severe pain and discomfort. Some of the symptoms that many patients can experience include sharp pain at the time of the injury, bruising, swelling, and it is often difficult to walk. This type of injury can happen as a result of participating in running and jumping movements, or if a new activity begins suddenly. Effective treatments can include wearing a brace or cast as the healing process occurs, and in severe tears, surgery may be necessary. If you have pain in your calf, it is strongly advised that you speak to a podiatrist as quickly as possible who can treat an Achilles tendon injury.
The Achilles tendon connects the heel to the calf muscles. It is located in the back of the leg, near the foot, and is responsible for the ability to point and flex the foot. An injury can cause the Achilles tendon to become ruptured or injured, and this generally causes severe pain and discomfort. Some of the symptoms that many patients can experience include sharp pain at the time of the injury, bruising, swelling, and it is often difficult to walk. This type of injury can happen as a result of participating in running and jumping movements, or if a new activity begins suddenly. Effective treatments can include wearing a brace or cast as the healing process occurs, and in severe tears, surgery may be necessary. If you have pain in your calf, it is strongly advised that you speak to a podiatrist as quickly as possible who can treat an Achilles tendon injury.
Achilles tendon injuries need immediate attention to avoid future complications. If you have any concerns, contact Julie Jurd-Sadler, DPM of Progressive Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is the Achilles Tendon?
The Achilles tendon is a tendon that connects the lower leg muscles and calf to the heel of the foot. It is the strongest tendon in the human body and is essential for making movement possible. Because this tendon is such an integral part of the body, any injuries to it can create immense difficulties and should immediately be presented to a doctor.
What Are the Symptoms of an Achilles Tendon Injury?
There are various types of injuries that can affect the Achilles tendon. The two most common injuries are Achilles tendinitis and ruptures of the tendon.
Achilles Tendinitis Symptoms
- Inflammation
- Dull to severe pain
- Increased blood flow to the tendon
- Thickening of the tendon
Rupture Symptoms
- Extreme pain and swelling in the foot
- Total immobility
Treatment and Prevention
Achilles tendon injuries are diagnosed by a thorough physical evaluation, which can include an MRI. Treatment involves rest, physical therapy, and in some cases, surgery. However, various preventative measures can be taken to avoid these injuries, such as:
- Thorough stretching of the tendon before and after exercise
- Strengthening exercises like calf raises, squats, leg curls, leg extensions, leg raises, lunges, and leg presses
If you have any questions please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Plantar Warts Can Be Treated!
Why Do Cracked Heels Form?
 Having dry skin is one of the many factors that can result in the formation of cracked heels. Those who have biomechanical issues that increase the pressure put on the heel, may be more likely to experience cracked heels. Being obese can also create an increase in pressure put on the heels, as the feet are responsible to carry the extra weight. This causes a loss of suppleness in the pads of the feet. Due to this lack of flexibility and increased pressure, cracks and deep fissures can form on the heels. Wearing open back shoes can also be a risk factor for developing cracked heels, as these types of shoes may cause the fat pads in the heel to expand sideways, creating cracks. Certain skin conditions, such as psoriasis, eczema, and fungal infections, can increase dryness of the skin thus leading to cracks or fissures. In severe cases, cracked heels may cause bleeding. If you feel you have developed cracked heels, please visit a podiatrist for professional care and treatment.
Having dry skin is one of the many factors that can result in the formation of cracked heels. Those who have biomechanical issues that increase the pressure put on the heel, may be more likely to experience cracked heels. Being obese can also create an increase in pressure put on the heels, as the feet are responsible to carry the extra weight. This causes a loss of suppleness in the pads of the feet. Due to this lack of flexibility and increased pressure, cracks and deep fissures can form on the heels. Wearing open back shoes can also be a risk factor for developing cracked heels, as these types of shoes may cause the fat pads in the heel to expand sideways, creating cracks. Certain skin conditions, such as psoriasis, eczema, and fungal infections, can increase dryness of the skin thus leading to cracks or fissures. In severe cases, cracked heels may cause bleeding. If you feel you have developed cracked heels, please visit a podiatrist for professional care and treatment.
Cracked heels are unsightly and can cause further damage to your shoes and feet. If you have any concerns, contact Julie Jurd-Sadler, DPM from Progressive Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Cracked Heels
Cracked heels appear unappealing and can make it harder for you walk around in sandals. Aside from looking unpleasant, cracked heels can also tear stockings, socks, and wear out your shoes. There are several methods to help restore a cracked heel and prevent further damage.
How Do You Get Them?
Dry skin is the number one culprit in creating cracked heels. Many athletes, walkers, joggers, and even swimmers suffer from cracked heels. Age and skin oil production play a role to getting cracked heels as well.
Promote Healing
Over the counter medicines can help, especially for those that need instant relief or who suffer from chronic dry feet.
Wear Socks – Wearing socks with medicated creams helps lock in moisture.
Moisturizers – Applying both day and night will help alleviate dryness which causes cracking.
Pumice Stones – These exfoliate and remove dead skin, which allows for smoother moisturizer application and better absorption into the skin.
Change in Diet
Eating healthy with a well-balanced diet will give the skin a fresh and radiant look. Your body responds to the kinds of food you ingest. Omega-3 fatty acids and zinc supplements can also revitalize skin tissue.
Most importantly, seek professional help if unsure how to proceed in treating cracked heels. A podiatrist will help you with any questions or information needed.
If you have any questions, please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
More...
Heel Spur Symptoms
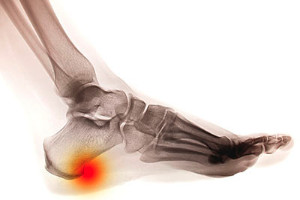 Patients who experience heel pain may be aware that this can be indicative of a heel spur. This is defined as a small piece of bone that grows on the inside of the heel and is often confused with plantar fasciitis. It can develop from a strained plantar fascia, which may be a result of wearing shoes that do not fit correctly. Common symptoms that often accompany heel spurs include pain and discomfort in the heel and surrounding areas, and it is often difficult to perform daily activities. Patients may find comfort in practicing specific foot stretches that can help to relax the tissues near the heel, and relief may be found when the affected foot is rested and elevated. It is strongly advised that you consult with a podiatrist who can determine the cause of existing heel pain, and offer correct treatment options for heel spurs.
Patients who experience heel pain may be aware that this can be indicative of a heel spur. This is defined as a small piece of bone that grows on the inside of the heel and is often confused with plantar fasciitis. It can develop from a strained plantar fascia, which may be a result of wearing shoes that do not fit correctly. Common symptoms that often accompany heel spurs include pain and discomfort in the heel and surrounding areas, and it is often difficult to perform daily activities. Patients may find comfort in practicing specific foot stretches that can help to relax the tissues near the heel, and relief may be found when the affected foot is rested and elevated. It is strongly advised that you consult with a podiatrist who can determine the cause of existing heel pain, and offer correct treatment options for heel spurs.
Heel spurs can be incredibly painful and sometimes may make you unable to participate in physical activities. To get medical care for your heel spurs, contact Julie Jurd-Sadler, DPM from Progressive Podiatry. Our doctor will do everything possible to treat your condition.
Heels Spurs
Heel spurs are formed by calcium deposits on the back of the foot where the heel is. This can also be caused by small fragments of bone breaking off one section of the foot, attaching onto the back of the foot. Heel spurs can also be bone growth on the back of the foot and may grow in the direction of the arch of the foot.
Older individuals usually suffer from heel spurs and pain sometimes intensifies with age. One of the main condition's spurs are related to is plantar fasciitis.
Pain
The pain associated with spurs is often because of weight placed on the feet. When someone is walking, their entire weight is concentrated on the feet. Bone spurs then have the tendency to affect other bones and tissues around the foot. As the pain continues, the feet will become tender and sensitive over time.
Treatments
There are many ways to treat heel spurs. If one is suffering from heel spurs in conjunction with pain, there are several methods for healing. Medication, surgery, and herbal care are some options.
If you have any questions feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the latest in diagnostic and treatment technology to meet your needs.
Rheumatoid Arthritis and the Feet
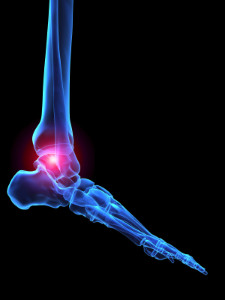 Rheumatoid arthritis is an inflammatory form of arthritis that can create complications with the feet. This condition may cause swelling within the joints of the feet, making it very painful to complete daily tasks. Other symptoms include joint stiffness, fatigue, muscle pain, and numbness. Some risk factors for developing rheumatoid arthritis include genetics, bacteria and viruses, physical trauma, and obesity. In order to treat this condition, it may be beneficial to visit a doctor for prescribed medication, partake in physical therapy, and in more severe cases, surgery. It’s been said that having a well balanced diet may help relieve some of the symptoms associated with this condition. For a proper diagnosis and advised treatment plan, it’s suggested that you consult with a podiatrist for professional care.
Rheumatoid arthritis is an inflammatory form of arthritis that can create complications with the feet. This condition may cause swelling within the joints of the feet, making it very painful to complete daily tasks. Other symptoms include joint stiffness, fatigue, muscle pain, and numbness. Some risk factors for developing rheumatoid arthritis include genetics, bacteria and viruses, physical trauma, and obesity. In order to treat this condition, it may be beneficial to visit a doctor for prescribed medication, partake in physical therapy, and in more severe cases, surgery. It’s been said that having a well balanced diet may help relieve some of the symptoms associated with this condition. For a proper diagnosis and advised treatment plan, it’s suggested that you consult with a podiatrist for professional care.
Arthritis can be a difficult condition to live with. If you are seeking treatment, contact Julie Jurd-Sadler, DPM from Progressive Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Arthritic Foot Care
Arthritis is a term that is commonly used to describe joint pain. The condition itself can occur to anyone of any age, race, or gender, and there are over 100 types of it. Nevertheless, arthritis is more commonly found in women compared to men, and it is also more prevalent in those who are overweight. The causes of arthritis vary depending on which type of arthritis you have. Osteoarthritis for example, is often caused by injury, while rheumatoid arthritis is caused by a misdirected immune system.
Symptoms
- Swelling
- Pain
- Stiffness
- Decreased Range of Motion
Arthritic symptoms range in severity, and they may come and go. Some symptoms stay the same for several years but could potentially get worse with time. Severe cases of arthritis can prevent its sufferers from performing daily activities and make walking difficult.
Risk Factors
- Occupation – Occupations requiring repetitive knee movements have been linked to osteoarthritis
- Obesity – Excess weight can contribute to osteoarthritis development
- Infection – Microbial agents can infect the joints and trigger arthritis
- Joint Injuries – Damage to joints may lead to osteoarthritis
- Age – Risk increases with age
- Gender –Most types are more common in women
- Genetics – Arthritis can be hereditary
If you suspect your arthritis is affecting your feet, it is crucial that you see a podiatrist immediately. Your doctor will be able to address your specific case and help you decide which treatment method is best for you.
If you have any questions, please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
How Does Plantar Hyperhidrosis Occur?
 Hyperhidrosis is the medical term that is used to define excessive sweating. Some patients have feet that sweat for the majority of the day, and this is referred to as plantar hyperhidrosis. It may happen as a result of anxiety, hormonal changes, or living in a hot environment. This condition may cause embarrassment during the day as the feet begin to slide in certain types of shoes. Additionally, rashes may develop, and there may be an odor coming from the feet. It is beneficial to wear shoes that are made of breathable materials, and comfort may be found when foot powder is frequently sprinkled in the shoes. If you have symptoms of plantar hyperhidrosis, it is strongly suggested that you consult with a podiatrist who can help you to manage this condition.
Hyperhidrosis is the medical term that is used to define excessive sweating. Some patients have feet that sweat for the majority of the day, and this is referred to as plantar hyperhidrosis. It may happen as a result of anxiety, hormonal changes, or living in a hot environment. This condition may cause embarrassment during the day as the feet begin to slide in certain types of shoes. Additionally, rashes may develop, and there may be an odor coming from the feet. It is beneficial to wear shoes that are made of breathable materials, and comfort may be found when foot powder is frequently sprinkled in the shoes. If you have symptoms of plantar hyperhidrosis, it is strongly suggested that you consult with a podiatrist who can help you to manage this condition.
If you are suffering from hyperhidrosis contact Julie Jurd-Sadler, DPM of Progressive Podiatry. Our doctor can provide the care you need to attend to all of your foot and ankle needs.
Hyperhidrosis of the Feet
Hyperhidrosis is a rare disorder that can cause people to have excessive sweating of their feet. This can usually occur all on its own without rigorous activity involved. People who suffer from hyperhidrosis may also experience sweaty palms.
Although it is said that sweating is a healthy process meant to cool down the body temperature and to maintain a proper internal temperature, hyperhidrosis may prove to be a huge hindrance on a person’s everyday life.
Plantar hyperhidrosis is considered to be the main form of hyperhidrosis. Secondary hyperhidrosis can refer to sweating that occurs in areas other than the feet or hands and armpits. Often this may be a sign of it being related to another medical condition such as menopause, hyperthyroidism and even Parkinson’s disease.
In order to alleviate this condition, it is important to see your doctor so that they may prescribe the necessary medications so that you can begin to live a normal life again. If this is left untreated, it is said that it will persist throughout an individual’s life.
A last resort approach would be surgery, but it is best to speak with your doctor to find out what may be the best treatment for you.
If you have any questions please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Do You Suffer From Painful Feet?
Blog Archives
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019