Connect With Us
Blog
Items filtered by date: October 2020
Did I Fracture My Foot?
 A broken foot can occur as a simple crack or as a complete break in the bone. Signs of a fractured foot can include tenderness, increased pain when standing or walking, numbness, swelling, bruising, trouble with movement, and an abnormal foot shape. If you believe that you have fractured your foot, you will likely need to visit a podiatrist for a proper diagnosis. In order to properly diagnose a foot fracture, an X-ray, CT scan, MRI or a bone scan will be necessary. Once a foot fracture is diagnosed, a cast, splint, or boot may be needed to limit the foot’s movement. A podiatrist will likely prescribe medicine, and in some cases surgery may be necessary as well.
A broken foot can occur as a simple crack or as a complete break in the bone. Signs of a fractured foot can include tenderness, increased pain when standing or walking, numbness, swelling, bruising, trouble with movement, and an abnormal foot shape. If you believe that you have fractured your foot, you will likely need to visit a podiatrist for a proper diagnosis. In order to properly diagnose a foot fracture, an X-ray, CT scan, MRI or a bone scan will be necessary. Once a foot fracture is diagnosed, a cast, splint, or boot may be needed to limit the foot’s movement. A podiatrist will likely prescribe medicine, and in some cases surgery may be necessary as well.
A broken foot requires immediate medical attention and treatment. If you need your feet checked, contact Julie Jurd-Sadler, DPM from Progressive Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Broken Foot Causes, Symptoms, and Treatment
A broken foot is caused by one of the bones in the foot typically breaking when bended, crushed, or stretched beyond its natural capabilities. Usually the location of the fracture indicates how the break occurred, whether it was through an object, fall, or any other type of injury.
Common Symptoms of Broken Feet:
- Bruising
- Pain
- Redness
- Swelling
- Blue in color
- Numbness
- Cold
- Misshapen
- Cuts
- Deformities
Those that suspect they have a broken foot shoot seek urgent medical attention where a medical professional could diagnose the severity.
Treatment for broken bones varies depending on the cause, severity and location. Some will require the use of splints, casts or crutches while others could even involve surgery to repair the broken bones. Personal care includes the use of ice and keeping the foot stabilized and elevated.
If you have any questions please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
What to Do During a Gout Attack
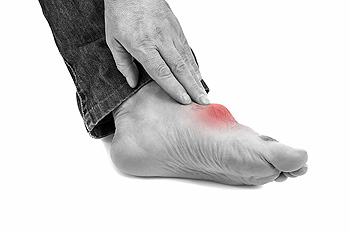 Excess levels of uric acid in the blood may lead to the medical condition that is known as gout. Crystals can form in the joints of the big toe, and this can cause severe pain and discomfort. Additional symptoms that patients experience may consist of swelling, heat and redness, and it may become difficult to walk. Gout is considered to be a form of arthritis and it can develop for a variety of reasons. These can include genetic factors, eating foods that have high purine levels, or from taking certain medications. When a gout attack occurs it can be beneficial to rest and elevate the affected foot, as well as apply ice packs and take anti-inflammatory medication, and the pain may be reduced. Gout can be a debilitating foot condition, which is why you should consult with a podiatrist as quickly as possible so correct treatment options can be discussed.
Excess levels of uric acid in the blood may lead to the medical condition that is known as gout. Crystals can form in the joints of the big toe, and this can cause severe pain and discomfort. Additional symptoms that patients experience may consist of swelling, heat and redness, and it may become difficult to walk. Gout is considered to be a form of arthritis and it can develop for a variety of reasons. These can include genetic factors, eating foods that have high purine levels, or from taking certain medications. When a gout attack occurs it can be beneficial to rest and elevate the affected foot, as well as apply ice packs and take anti-inflammatory medication, and the pain may be reduced. Gout can be a debilitating foot condition, which is why you should consult with a podiatrist as quickly as possible so correct treatment options can be discussed.
Gout is a painful condition that can be treated. If you are seeking treatment, contact Julie Jurd-Sadler, DPM from Progressive Podiatry. Our doctor will treat your foot and ankle needs.
What Is Gout?
Gout is a form of arthritis that is characterized by sudden, severe attacks of pain, redness, and tenderness in the joints. The condition usually affects the joint at the base of the big toe. A gout attack can occur at any random time, such as the middle of the night while you are asleep.
Symptoms
- Intense Joint Pain - Usually around the large joint of your big toe, and it most severe within the first four to twelve hours
- Lingering Discomfort - Joint discomfort may last from a few days to a few weeks
- Inflammation and Redness -Affected joints may become swollen, tender, warm and red
- Limited Range of Motion - May experience a decrease in joint mobility
Risk Factors
- Genetics - If family members have gout, you’re more likely to have it
- Medications - Diuretic medications can raise uric acid levels
- Gender/Age - Gout is more common in men until the age of 60. It is believed that estrogen protects women until that point
- Diet - Eating red meat and shellfish increases your risk
- Alcohol - Having more than two alcoholic drinks per day increases your risk
- Obesity - Obese people are at a higher risk for gout
Prior to visiting your podiatrist to receive treatment for gout, there are a few things you should do beforehand. If you have gout you should write down your symptoms--including when they started and how often you experience them, important medical information you may have, and any questions you may have. Writing down these three things will help your podiatrist in assessing your specific situation so that he or she may provide the best route of treatment for you.
If you have any questions, please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Where Is the Tarsal Tunnel Located?
 The tibial nerve is located in a small tunnel surrounded by tendons in the inner side of the ankle. Tarsal tunnel syndrome can develop when this specific nerve becomes compressed, and is often accompanied by pain and swelling. It may happen as a result of enduring an ankle injury, such as a sprain or fracture, or from having bone spurs. Mild relief may be found when the affected foot is elevated, and it may help to take anti-inflammatory medication. In severe cases, surgery can be a viable option to permanently reduce or eliminate the pain that is associated with this condition. If you have developed this ailment, it is strongly recommended that you speak with a podiatrist who can help you choose the correct treatment option.
The tibial nerve is located in a small tunnel surrounded by tendons in the inner side of the ankle. Tarsal tunnel syndrome can develop when this specific nerve becomes compressed, and is often accompanied by pain and swelling. It may happen as a result of enduring an ankle injury, such as a sprain or fracture, or from having bone spurs. Mild relief may be found when the affected foot is elevated, and it may help to take anti-inflammatory medication. In severe cases, surgery can be a viable option to permanently reduce or eliminate the pain that is associated with this condition. If you have developed this ailment, it is strongly recommended that you speak with a podiatrist who can help you choose the correct treatment option.
Tarsal tunnel syndrome can be very uncomfortable to live with. If you are experiencing tarsal tunnel syndrome, contact Julie Jurd-Sadler, DPM of Progressive Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Tarsal Tunnel Syndrome
Tarsal tunnel syndrome, which can also be called tibial nerve dysfunction, is an uncommon condition of misfiring peripheral nerves in the foot. The tibial nerve is the peripheral nerve in the leg responsible for sensation and movement of the foot and calf muscles. In tarsal tunnel syndrome, the tibial nerve is damaged, causing problems with movement and feeling in the foot of the affected leg.
Common Cause of Tarsal Tunnel Syndrome
- Involves pressure or an injury, direct pressure on the tibial nerve for an extended period of time, sometimes caused by other body structures close by or near the knee.
- Diseases that damage nerves, including diabetes, may cause tarsal tunnel syndrome.
- At times, tarsal tunnel syndrome can appear without an obvious cause in some cases.
The Effects of Tarsal Tunnel Syndrome
- Different sensations, an afflicted person may experience pain, tingling, burning or other unusual sensations in the foot of the affected leg.
- The foot muscles, toes and ankle become weaker, and curling your toes or flexing your foot can become difficult.
- If condition worsens, infections and ulcers may develop on the foot that is experiencing the syndrome.
A physical exam of the leg can help identify the presence of tarsal tunnel syndrome. Medical tests, such as a nerve biopsy, are also used to diagnose the condition. Patients may receive physical therapy and prescriptive medication. In extreme cases, some may require surgery.
If you have any questions please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
What Are the Treatments for Plantar Fasciitis?
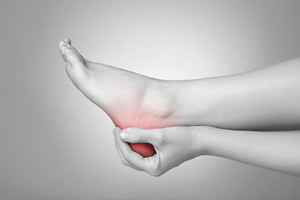 Plantar fasciitis, a condition that causes pain in the heel and bottom of the foot, is common and has many different treatments. Resting the foot limits its movements and allows time for healing. Icing the foot can decrease pain and swelling, as can taking nonsteroidal anti-inflammatory medications. For when you need to be on your feet, orthotic shoe inserts can help cushion and support your foot. Doing certain stretches and strengthening exercises can increase the flexibility of your feet and make the plantar fascia stronger, thereby decreasing pain. In rarer cases, when conservative treatments have failed and pain interferes significantly with daily activities, surgery may become an option. To discover the best treatment options for you, seek the care of a podiatrist.
Plantar fasciitis, a condition that causes pain in the heel and bottom of the foot, is common and has many different treatments. Resting the foot limits its movements and allows time for healing. Icing the foot can decrease pain and swelling, as can taking nonsteroidal anti-inflammatory medications. For when you need to be on your feet, orthotic shoe inserts can help cushion and support your foot. Doing certain stretches and strengthening exercises can increase the flexibility of your feet and make the plantar fascia stronger, thereby decreasing pain. In rarer cases, when conservative treatments have failed and pain interferes significantly with daily activities, surgery may become an option. To discover the best treatment options for you, seek the care of a podiatrist.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Julie Jurd-Sadler, DPM from Progressive Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
- Excessive running
- Non-supportive shoes
- Overpronation
- Repeated stretching and tearing of the plantar fascia
How Can It Be Treated?
- Conservative measures – anti-inflammatories, ice packs, stretching exercises, physical therapy, orthotic devices
- Shockwave therapy – sound waves are sent to the affected area to facilitate healing and are usually used for chronic cases of plantar fasciitis
- Surgery – usually only used as a last resort when all else fails. The plantar fascia can be surgically detached from the heel
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Blog Archives
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019