Connect With Us
Blog
Blog
Diagnosing an Achilles Tendon Rupture

An Achilles tendon rupture often presents suddenly, typically accompanied by a sharp pain in the back of the leg and sometimes an audible snapping sound. Many people with this injury mistakenly believe they have been hit in the calf. When examining for an Achilles rupture, the presence of swelling and bruising varies and is not entirely reliable. The gap in the tendon that indicates a rupture is often not easily palpable due to local swelling. In terms of mobility, patients can usually still perform some active movement in the ankle because other tendons also connect the calf to the foot. Pain affects passive movement but does not always limit it. Despite a ruptured Achilles, those affected can often still walk and may even be able to stand on tiptoes when using both feet, though not on the injured limb alone. The Simmonds' calf squeeze test is a reliable way for podiatrists to check for an Achilles tendon rupture. The test is done by having the patient kneel or lie prone with dangling feet. The healthy calf is used to see the foot flex, while no movement on the injured side indicates a ruptured Achilles tendon. If you believe you may have injured your Achilles tendon, it is strongly suggested that you make an appointment with a podiatrist for a thorough evaluation, diagnosis, and appropriate treatment.
Achilles tendon injuries need immediate attention to avoid future complications. If you have any concerns, contact Julie Jurd-Sadler, DPM of Progressive Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is the Achilles Tendon?
The Achilles tendon is a tendon that connects the lower leg muscles and calf to the heel of the foot. It is the strongest tendon in the human body and is essential for making movement possible. Because this tendon is such an integral part of the body, any injuries to it can create immense difficulties and should immediately be presented to a doctor.
What Are the Symptoms of an Achilles Tendon Injury?
There are various types of injuries that can affect the Achilles tendon. The two most common injuries are Achilles tendinitis and ruptures of the tendon.
Achilles Tendinitis Symptoms
- Inflammation
- Dull to severe pain
- Increased blood flow to the tendon
- Thickening of the tendon
Rupture Symptoms
- Extreme pain and swelling in the foot
- Total immobility
Treatment and Prevention
Achilles tendon injuries are diagnosed by a thorough physical evaluation, which can include an MRI. Treatment involves rest, physical therapy, and in some cases, surgery. However, various preventative measures can be taken to avoid these injuries, such as:
- Thorough stretching of the tendon before and after exercise
- Strengthening exercises like calf raises, squats, leg curls, leg extensions, leg raises, lunges, and leg presses
If you have any questions please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Benefits of MLS Laser Therapy
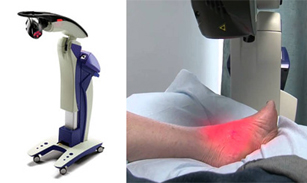
Whether you are dealing with chronic discomfort, the aftermath of an injury, or the wear and tear of daily life, Multiwave Locked System, or MLS, laser therapy may be a solution. MLS laser therapy is a non-invasive approach to foot pain. It aids in recovery from a variety of foot ailments, including sports injuries, arthritic pain, and nerve pain from diabetes, as well as heel pain from plantar fasciitis and Achilles tendon injuries. It has also been helpful in dealing with wounds that will not heal. MLS laser therapy does not involve medication, needles, or surgery and is FDA-approved for both safety and effectiveness. Furthermore, MLS laser therapy addresses the challenge of inflammation, a common hindrance to mobility and a source of discomfort in podiatric conditions. It actively reduces inflammation, decreasing pain and increasing comfort. MLS laser therapy not only accelerates the healing process but also allows for treatment plans that cater to specific foot care needs. To determine if MLS laser therapy is right for you, it is suggested that you consult a podiatrist.
MLS Laser Therapy is a successful alternative for treating any pain you may be experiencing related to certain podiatric conditions. If you are interested in MLS Laser Therapy, consult with Julie Jurd-Sadler, DPM from Progressive Podiatry. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
MLS Laser Therapy
Multiwave Locked System (MLS) Laser Therapy is a patented, FDA-cleared technology that helps relieve pain and inflammation from a number of podiatric conditions, including:
- Heel Pain
- Plantar Fasciitis
- Sports Injuries
- Wounds
- Achilles Tendonitis
- Arthritis
- Neuropathy
- Neuromas
MLS Laser Therapy is an ideal alternative to surgery and prescription medication, as it has no negative side effects and encourages accelerated healing. Among its many clinical benefits, MLS Laser Therapy also:
- Reduces swelling due to bruising or inflammation
- Blocks pain
- Reduces formation of scar tissue
- Improves nerve function
If you have any questions, please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Gout Pain Can Be Managed
Treatment Options for Bunionettes
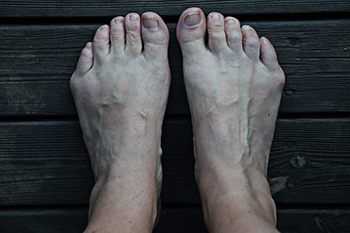
Tailor's bunion, also known as a bunionette, is a painful condition that develops on the outer side of the foot, specifically over the fifth metatarsophalangeal joint, or the 5th MPJ. This condition causes pressure pain, the formation of painful calluses, and difficulty when wearing shoes. One cause of tailor's bunion is a biomechanical abnormality where changes in your foot’s structure gradually cause the metatarsal bones to separate and a bunion to form. Conservative treatment options include padding, footwear modification, and custom-made orthotics. This condition is progressive and generally does not improve on its own. Surgical options include ostectomy, which removes the painful bump from the head of the fifth metatarsal. This type of surgery involves cutting the fifth metatarsal bone and realigning it. Surgical intervention may also include the removal of a painful bursa, if present. If tailor's bunion significantly hinders daily activities, causes discomfort while wearing shoes, or leads to excessive pain, it is suggested that you make an appointment with a podiatrist who can determine what the most appropriate course of action is.
If you are suffering from bunions, contact Julie Jurd-Sadler, DPM of Progressive Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
A bunion is formed of swollen tissue or an enlargement of boney growth, usually located at the base joint of the toe that connects to the foot. The swelling occurs due to the bones in the big toe shifting inward, which impacts the other toes of the foot. This causes the area around the base of the big toe to become inflamed and painful.
Why Do Bunions Form?
Genetics – Susceptibility to bunions are often hereditary
Stress on the feet – Poorly fitted and uncomfortable footwear that places stress on feet, such as heels, can worsen existing bunions
How Are Bunions Diagnosed?
Doctors often perform two tests – blood tests and x-rays – when trying to diagnose bunions, especially in the early stages of development. Blood tests help determine if the foot pain is being caused by something else, such as arthritis, while x-rays provide a clear picture of your bone structure to your doctor.
How Are Bunions Treated?
- Refrain from wearing heels or similar shoes that cause discomfort
- Select wider shoes that can provide more comfort and reduce pain
- Anti-inflammatory and pain management drugs
- Orthotics or foot inserts
- Surgery
If you have any questions, please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Navigating Foot Pain and Discomfort From Morton’s Neuroma
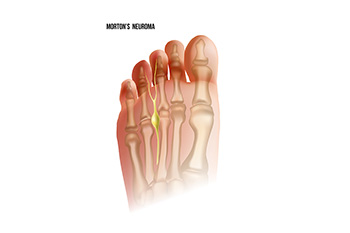
Morton's neuroma, a common and painful foot condition, affects the nerves in the ball of the foot, typically between the third and fourth toes. This ailment involves a thickening of the tissue around the nerve, causing sharp, burning pain, or a sensation that is similar to standing on a pebble or marble. It predominantly affects middle-aged women, but anyone can be susceptible. The exact cause is often associated with wearing tight or high-heeled shoes, which can compress the toes and aggravate the nerve. Other potential factors can include foot deformities or repetitive stress on the forefoot. The symptoms of Morton's neuroma can disrupt daily activities and diminish the quality of life. Treatments may range from changing footwear and utilizing orthotics to corticosteroid injections or, in severe cases, surgical removal of the affected nerve. If you have pain in this part of your foot, it is suggested that you seek professional advice from a podiatrist who can provide timely treatment that can manage the condition, alleviate pain, and restore comfort in your daily stride.
Morton’s neuroma is a very uncomfortable condition to live with. If you think you have Morton’s neuroma, contact Julie Jurd-Sadler, DPM of Progressive Podiatry. Our doctor will attend to all of your foot care needs and answer any of your related questions.
Morton’s Neuroma
Morton's neuroma is a painful foot condition that commonly affects the areas between the second and third or third and fourth toe, although other areas of the foot are also susceptible. Morton’s neuroma is caused by an inflamed nerve in the foot that is being squeezed and aggravated by surrounding bones.
What Increases the Chances of Having Morton’s Neuroma?
- Ill-fitting high heels or shoes that add pressure to the toe or foot
- Jogging, running or any sport that involves constant impact to the foot
- Flat feet, bunions, and any other foot deformities
Morton’s neuroma is a very treatable condition. Orthotics and shoe inserts can often be used to alleviate the pain on the forefront of the feet. In more severe cases, corticosteroids can also be prescribed. In order to figure out the best treatment for your neuroma, it’s recommended to seek the care of a podiatrist who can diagnose your condition and provide different treatment options.
If you have any questions, please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Detrimental Effects of Wearing High Heels

High heels are a popular fashion choice, often adding a stylish touch to special occasions. However, one should be aware of the potential negative effects on foot health when worn regularly. High heels can lead to various foot problems, including bunions, blisters, corns, and calluses. One common side effect is lower back pain, as these shoes lack adequate foot support, causing an uneven weight distribution. Foot pain is prevalent due to circulation problems and metatarsalgia. Ankle sprains, broken ankles, and awkward spinal curvature may result from wearing high heels, especially on uneven surfaces. Furthermore, high heels can constrict blood vessels and hinder natural blood flow, potentially leading to varicose veins and deformities such as hammertoe. They can also weaken ligaments and increase pressure on the knee joint, possibly causing osteoarthritis. If you enjoy wearing high heels, it is suggested that you make an appointment with a podiatrist to discuss the frequency of wear and consider alternative footwear choices that may help prevent potential health issues.
High heels have a history of causing foot and ankle problems. If you have any concerns about your feet or ankles, contact Julie Jurd-Sadler, DPM from Progressive Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Effects of High Heels on the Feet
High heels are popular shoes among women because of their many styles and societal appeal. Despite this, high heels can still cause many health problems if worn too frequently.
Which Parts of My Body Will Be Affected by High Heels?
- Ankle Joints
- Achilles Tendon – May shorten and stiffen with prolonged wear
- Balls of the Feet
- Knees – Heels cause the knees to bend constantly, creating stress on them
- Back – They decrease the spine’s ability to absorb shock, which may lead to back pain. The vertebrae of the lower back may compress.
What Kinds of Foot Problems Can Develop from Wearing High Heels?
- Corns
- Calluses
- Hammertoe
- Bunions
- Morton’s Neuroma
- Plantar Fasciitis
How Can I Still Wear High Heels and Maintain Foot Health?
If you want to wear high heeled shoes, make sure that you are not wearing them every day, as this will help prevent long term physical problems. Try wearing thicker heels as opposed to stilettos to distribute weight more evenly across the feet. Always make sure you are wearing the proper shoes for the right occasion, such as sneakers for exercising. If you walk to work, try carrying your heels with you and changing into them once you arrive at work. Adding inserts to your heels can help cushion your feet and absorb shock. Full foot inserts or metatarsal pads are available.
If you have any questions please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Fencing and Foot and Ankle Injuries

Fencing is a thrilling dance of swords, a clash of sharp intellects, and a showcase of exceptional skills. However, within the fluidity of each swift lunge and precise comeback, the potential for injuries lurks in the shadows. It can help to be aware of early indicators of injuries in fencing to proactively try to evade them. Foot and ankle injuries such as sprains and strains can emerge from absorbing the impact of swift maneuvers and changes in direction. Typical signs encompass discomfort, swelling, and challenges in walking or bearing weight. Safeguard against foot injuries by investing in top-tier fencing footwear, executing thorough warm-up routines, and upholding precise footwork techniques. In cases of foot injuries, the recommended course of action is resting, elevating, and compressing the affected limb. If you participate in fencing and have sustained a severe or persistent foot or ankle injury, it is suggested that you make an appointment with a podiatrist for a proper diagnosis and treatment.
Ankle and foot injuries are common among athletes and in many sports. They can be caused by several problems and may be potentially serious. If you are feeling pain or think you were injured in a sporting event or when exercising, consult with Julie Jurd-Sadler, DPM from Progressive Podiatry. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Common Injuries
The most common injuries that occur in sporting activities include:
- Achilles Tendonitis
- Achilles Tendon Rupture
- Ankle Sprains
- Broken Foot
- Plantar Fasciitis
- Stress Fractures
- Turf Toe
Symptoms
Symptoms vary depending upon the injury and in some cases, there may be no symptoms at all. However, in most cases, some form of symptom is experienced. Pain, aching, burning, bruising, tenderness, tightness or stiffness, sensation loss, difficulty moving, and swelling are the most common symptoms.
Treatment
Just as symptoms vary depending upon the injury, so do treatment options. A common treatment method is known as the RICE method. This method involves rest, applying ice, compression and elevating the afflicted foot or ankle. If the injury appears to be more serious, surgery might be required, such as arthroscopic or reconstructive surgery. Lastly, rehabilitation or therapy might be needed to gain full functionality in the afflicted area. Any discomfort experienced by an athlete must be evaluated by a licensed, reputable medical professional.
If you have any questions, please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Are You Suffering From Ingrown Toenails?
Alternative Treatment for Toenail Fungus
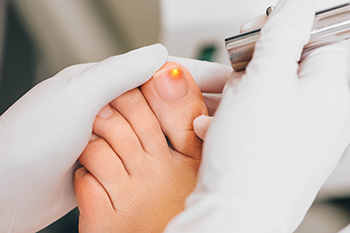
Toenail fungal infections, known as onychomycosis, are typically treated with antifungal medications. This type of infection is hard to cure. A complete cure of toenail fungus is considered an eradication of the fungus and a healthy-looking toenail. Lasers are being used to treat these infections and are being considered as an alternative treatment worthy of consideration. This may be particularly true among older patients, or those with health conditions that make traditional antifungal medications unsuitable or ineffective. If you have toenail fungus and it is not responding to antifungal medicines, it is suggested that you make an appointment with a podiatrist to discuss whether laser treatment may be correct for you.
Laser treatment can be an effective way to get rid of toenail fungus. If you have any questions about laser treatment, consult with Julie Jurd-Sadler, DPM from Progressive Podiatry. Our doctor will assess your condition and provide you with quality treatment for fungal nails.
What Are Toenail Fungal Infections?
Onychomycosis, or fungal infection of the nail, is a relatively common and non-serious condition. Around 10 percent of U.S. citizens are afflicted with fungal nails. Common forms of fungus that infect the nail include dermatophytes, yeasts, and molds.
Symptoms of Toenail Fungal Infections Include:
- Nail thickening
- Brittleness of the nail
- Discoloration of the nail
Diagnosis for Fungal Nails
Fungal infections are diagnosed by fungal culture and microscopy. This will rule out any other conditions such as nail trauma, psoriasis, lichen planus, and onychogryphosis.
What Is Laser Treatment?
Laser treatment is a non-invasive, safe, quick, and painless procedure that uses the heat from a laser to kill fungus in the nail. Each infected nail is targeted with a laser for several minutes. The treatment is usually utilized several different times over a select period. During this time, a podiatrist will keep an eye on the infection.
If you have any questions, please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
What to Do About Toe Cramps

Toe cramps can be painful as well as extremely annoying, especially when they wake you out of a sound sleep. Most cases of toe cramps are believed to be the result of overuse. Common culprits include walking too long, working out too much, and wearing shoes that force your feet to flex too much. Other causes of toe cramps include dehydration, along with consuming too much salt. Toe cramps also may be the result of deficiencies in such minerals as potassium, magnesium, and calcium. In addition, increased age, high anxiety, and other underlying medical conditions have been known to cause toe cramps. If you have toe cramps, it is suggested that you massage the area while trying to move the toes as much as you can. Also, applying a heating pad to the area for about 10 minutes can help. Be sure to wear shoes that fit properly and don’t squeeze the toes. Avoid sandals and flip-flops that cause the toes to flex when walking. Stretch your toes frequently and massage them while resting. For more information on how to deal with toe cramping, please consult a podiatrist.
Toe pain can disrupt your daily activities. If you have any concerns, contact Julie Jurd-Sadler, DPM of Progressive Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Causes Toe Pain?
Most severe toe pain is caused due to a sports injury, trauma from dropping something heavy on the toe, or bumping into something rigid. Other problems can develop over time for various reasons.
Toe pain can be caused by one or more ailments. The most common include:
- Trauma
- Sports injury
- Wearing shoes that are too tight
- Arthritis
- Gout
- Corns and calluses
- Hammertoe
- Bunions
- Blisters
- Ingrown toenails
- Sprains
- Fractures (broken bones)
- Dislocations
When to See a Podiatrist
- Severe pain
- Persistent pain that lasts more than a week
- Signs of infection
- Continued swelling
- Pain that prevents walking
Diagnosis
In many cases the cause of toe pain is obvious, but in others, a podiatrist may want to use more advanced methods to determine the problem. These can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatments for toe pain and injuries vary and may include shoe inserts, padding, taping, medicines, injections, and in some cases, surgery. If you believe that you have broken a toe, please see a podiatrist as soon as possible.
If you have any questions please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
More...
Causes and Effective Remedies for Heel Pain
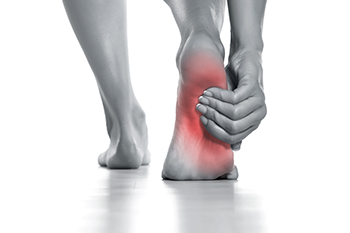
Heel pain is a common ailment that can disrupt daily life and activities. One of the primary culprits is plantar fasciitis, which occurs when the thick band of tissue known as the plantar fascia becomes inflamed or irritated. The plantar fascia is found on the bottom of the foot, and connects the heel to the toes. Plantar fasciitis often results from overuse, wearing improper footwear, or a sudden increase in physical activity. Another common cause of heel pain is Achilles tendonitis, which affects the Achilles tendon at the back of the heel, usually as a result of excessive strain or overuse. To alleviate heel pain, it is beneficial to rest and elevate the affected foot. Wearing proper footwear with adequate arch support can significantly help, in addition to wearing custom orthotic inserts. Performing stretching exercises for the calf muscles and Achilles tendon also can aid in recovery. In severe cases, surgical intervention may be necessary. If you are experiencing heel pain, it is strongly suggested that you make an appointment with a podiatrist who can determine the cause and offer treatment options that are right for you.
Many people suffer from bouts of heel pain. For more information, contact Julie Jurd-Sadler, DPM of Progressive Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
- Wearing ill-fitting shoes
- Wearing non-supportive shoes
- Weight change
- Excessive running
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions please contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
How to Choose the Right Running Shoe

Choosing the perfect pair of running shoes is essential for runners of all levels. Your choice significantly affects comfort, performance, and overall foot health. To make the right selection, start by identifying your foot type, such as neutral, pronated, or supinated. Next, consider cushioning, which should be minimal for a natural feel, maximum for long-distance shock absorption, or moderate for most runners. Shoe stability matters for injury prevention. Those with flat feet or overpronation should opt for stability features like medial posts, while high arches benefit from neutral shoes with cushioning. A proper fit is also important. Leave about a thumb's width of space between your longest toe and the shoe's front. Try on multiple pairs and take them for a test run in-store to assess comfort and stability. Also, consider the type of surface you will be running on, because road, trail, and track running require different shoe types. Running shoes can become a major investment because they should be replaced after 300-500 miles to ensure optimal performance and prevent injuries. For more help with finding the proper running shoe for your feet, it is suggested that you speak to a podiatrist.
If you are a runner, wearing the right running shoe is essential. For more information, contact Julie Jurd-Sadler, DPM from Progressive Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Choosing the Right Running Shoe for Your Foot Type
To increase performance and avoid the risk of injury, it is important to choose the right running shoe based on your foot type. The general design of running shoes revolves around pronation, which is how the ankle rolls from outside to inside when the foot strikes the ground.
- Neutral runners are able to choose from a wide variety of shoes, including minimalist shoes or even going barefoot.
- Runners who overpronate, or experience an over-abundance of ankle rolling, should choose shoes that provide extra motion control and stability.
- Runners who underpronate, or supinate, have feet that have high arches and lack flexibility, preventing shock absorption. They require shoes with more flexibility and cushion.
If you have any questions please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Causes and Types of Gout
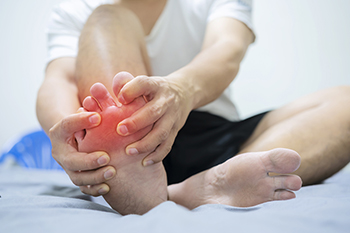
Gout, a form of arthritis, is a painful condition that can strike suddenly and severely. It happens as a result of the accumulation of urate crystals in the joints and often leads to inflammation and intense discomfort. Primary gout results from genetic factors. This can cause the body's overproduction of uric acid or a decreased ability to excrete it, which can affect joints like the ankle and big toe. Secondary gout is caused by underlying conditions, such as kidney disease, hypertension, or obesity. These hinder the body's ability to manage uric acid levels. Gout that occurs suddenly in a single joint is referred to as acute gout and generally affects the big toe. This form of gout is characterized by excruciating pain, redness, and swelling. If left untreated, acute gout can progress into chronic gout and lead to recurrent, long-lasting joint pain and deformities. Identifying the specific type and underlying causes of gout is essential for devising an effective treatment plan, which may include lifestyle changes, medications, and dietary adjustments. If you have had one or frequent gout attacks, it is strongly suggested that you are under the care of a podiatrist. This type of doctor can accurately determine which type of gout is present and offer the correct treatment methods.
Gout is a painful condition that can be treated. If you are seeking treatment, contact Julie Jurd-Sadler, DPM from Progressive Podiatry. Our doctor will treat your foot and ankle needs.
What Is Gout?
Gout is a form of arthritis that is characterized by sudden, severe attacks of pain, redness, and tenderness in the joints. The condition usually affects the joint at the base of the big toe. A gout attack can occur at any random time, such as the middle of the night while you are asleep.
Symptoms
- Intense Joint Pain - Usually around the large joint of your big toe, and it most severe within the first four to twelve hours
- Lingering Discomfort - Joint discomfort may last from a few days to a few weeks
- Inflammation and Redness -Affected joints may become swollen, tender, warm and red
- Limited Range of Motion - May experience a decrease in joint mobility
Risk Factors
- Genetics - If family members have gout, you’re more likely to have it
- Medications - Diuretic medications can raise uric acid levels
- Gender/Age - Gout is more common in men until the age of 60. It is believed that estrogen protects women until that point
- Diet - Eating red meat and shellfish increases your risk
- Alcohol - Having more than two alcoholic drinks per day increases your risk
- Obesity - Obese people are at a higher risk for gout
Prior to visiting your podiatrist to receive treatment for gout, there are a few things you should do beforehand. If you have gout you should write down your symptoms--including when they started and how often you experience them, important medical information you may have, and any questions you may have. Writing down these three things will help your podiatrist in assessing your specific situation so that he or she may provide the best route of treatment for you.
If you have any questions, please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Exploring Common Causes of Toe Pain
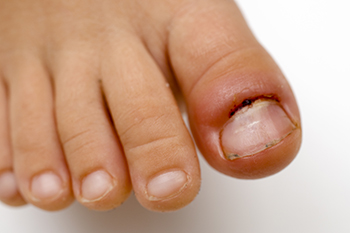
Our toes, those often overlooked companions on our daily journeys, play a more significant role in our lives than we realize, until they ache. Toe pain, a distressing sensation that can impede our daily activities, can arise from various sources. Wearing uncomfortable footwear, such as tight or ill-fitting shoes, may lead to blisters and calluses caused by excess friction. Stubbing a toe, seemingly harmless but potent in its impact, can result in acute pain and potential fractures. Ingrown toenails, a product of improper trimming or wearing shoes that do not fit correctly, can also trigger sharp, localized pain. Athlete's foot, a fungal infection, often targets the spaces between our toes, bringing about itchiness and discomfort. Arthritis can also affect the toes, leading to persistent toe pain. Acknowledging these common culprits empowers us to take better care of our toes, ensuring they continue to walk us through life's adventures without unnecessary pain. If you are experiencing toe pain, it is suggested that you confer with a podiatrist for proper treatment.
Toe pain can disrupt your daily activities. If you have any concerns, contact Julie Jurd-Sadler, DPM of Progressive Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Causes Toe Pain?
Most severe toe pain is caused due to a sports injury, trauma from dropping something heavy on the toe, or bumping into something rigid. Other problems can develop over time for various reasons.
Toe pain can be caused by one or more ailments. The most common include:
- Trauma
- Sports injury
- Wearing shoes that are too tight
- Arthritis
- Gout
- Corns and calluses
- Hammertoe
- Bunions
- Blisters
- Ingrown toenails
- Sprains
- Fractures (broken bones)
- Dislocations
When to See a Podiatrist
- Severe pain
- Persistent pain that lasts more than a week
- Signs of infection
- Continued swelling
- Pain that prevents walking
Diagnosis
In many cases the cause of toe pain is obvious, but in others, a podiatrist may want to use more advanced methods to determine the problem. These can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatments for toe pain and injuries vary and may include shoe inserts, padding, taping, medicines, injections, and in some cases, surgery. If you believe that you have broken a toe, please see a podiatrist as soon as possible.
If you have any questions please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Blog Archives
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019