Connect With Us
Blog
Blog
Understanding What Plantar Fasciitis Is

Plantar fasciitis is a common foot condition characterized by inflammation of the plantar fascia, a thick band of tissue that runs along the bottom of the foot, connecting the heel bone to the toes. This condition typically manifests as heel pain, particularly with the first steps in the morning or after periods of rest, which can gradually worsen throughout the day. The precise cause of plantar fasciitis is not always clear, but it often results from repetitive strain or excessive stress on the plantar fascia. Factors contributing to the development of plantar fasciitis include overuse from activities such as running, walking long distances, or standing for extended periods. Additionally, certain risk factors like obesity, high arches, flat feet, or tight calf muscles can increase the likelihood of developing plantar fasciitis. If you have heel pain, it is suggested that you visit a podiatrist who can effectively diagnose plantar fasciitis, and offer an appropriate treatment plan.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Julie Jurd-Sadler, DPM from Progressive Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
- Excessive running
- Non-supportive shoes
- Overpronation
- Repeated stretching and tearing of the plantar fascia
How Can It Be Treated?
- Conservative measures – anti-inflammatories, ice packs, stretching exercises, physical therapy, orthotic devices
- Shockwave therapy – sound waves are sent to the affected area to facilitate healing and are usually used for chronic cases of plantar fasciitis
- Surgery – usually only used as a last resort when all else fails. The plantar fascia can be surgically detached from the heel
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Causes and Nature of Morton's Neuroma
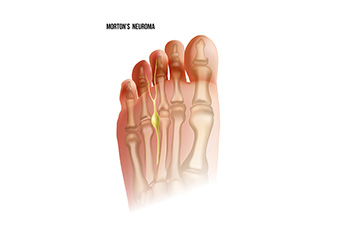
Morton's neuroma, a common foot condition, occurs when a nerve in the ball of the foot becomes thickened and inflamed, leading to pain and discomfort. This condition typically affects the area between the third and fourth toes but can also occur between other toes. The exact cause of Morton's neuroma is not always clear, but it often develops due to repetitive stress or irritation on the nerve, such as wearing tight or high-heeled shoes that compress the forefoot. Activities that involve repetitive pressure on the ball of the foot, such as running or participating in high-impact sports, can also contribute to the development of Morton's neuroma. Additionally, foot deformities like bunions, hammertoes, or flat feet may increase the risk. Understanding the underlying causes of Morton's neuroma is important for effective management and prevention strategies, which may include wearing supportive footwear, using orthotic inserts, and avoiding activities that exacerbate symptoms. If you have pain in this part of your foot, it is strongly suggested that you are under the care of a podiatrist who can accurately diagnose and treat Morton’s neuroma.
Morton’s neuroma is a very uncomfortable condition to live with. If you think you have Morton’s neuroma, contact Julie Jurd-Sadler, DPM of Progressive Podiatry. Our doctor will attend to all of your foot care needs and answer any of your related questions.
Morton’s Neuroma
Morton's neuroma is a painful foot condition that commonly affects the areas between the second and third or third and fourth toe, although other areas of the foot are also susceptible. Morton’s neuroma is caused by an inflamed nerve in the foot that is being squeezed and aggravated by surrounding bones.
What Increases the Chances of Having Morton’s Neuroma?
- Ill-fitting high heels or shoes that add pressure to the toe or foot
- Jogging, running or any sport that involves constant impact to the foot
- Flat feet, bunions, and any other foot deformities
Morton’s neuroma is a very treatable condition. Orthotics and shoe inserts can often be used to alleviate the pain on the forefront of the feet. In more severe cases, corticosteroids can also be prescribed. In order to figure out the best treatment for your neuroma, it’s recommended to seek the care of a podiatrist who can diagnose your condition and provide different treatment options.
If you have any questions, please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Understanding Foot Changes During Pregnancy

Pregnancy is marked by numerous changes in the body, including the feet. One notable alteration is the increase in shoe size experienced by many expectant mothers. This change occurs due to hormonal fluctuations and the body's natural tendency to retain fluids, which leads to swelling in the feet and ankles. Consequently, women may find that their usual shoe size feels snug or uncomfortable during pregnancy, necessitating the need for larger footwear to accommodate the swelling. Additionally, some pregnant individuals may encounter itching and redness on the soles of their feet, a condition known as pruritus gravidarum. This symptom can arise due to heightened blood circulation, hormonal changes, or skin stretching, causing discomfort and irritation. While these foot changes are a normal part of pregnancy, expectant mothers need to prioritize foot health by wearing supportive footwear, practicing gentle foot exercises, and elevating the feet to reduce swelling. Consulting with a podiatrist can also guide in managing foot discomfort and ensuring a smooth pregnancy journey. If you are seeking relief from foot conditions developed during pregnancy, it is suggested that you consult a podiatrist.
Pregnant women with swollen feet can be treated with a variety of different methods that are readily available. For more information about other cures for swollen feet during pregnancy, consult with Julie Jurd-Sadler, DPM from Progressive Podiatry. Our doctor will attend to all of your foot and ankle needs.
What Foot Problems Can Arise During Pregnancy?
One problem that can occur is overpronation, which occurs when the arch of the foot flattens and tends to roll inward. This can cause pain and discomfort in your heels while you’re walking or even just standing up, trying to support your baby.
Another problem is edema, or swelling in the extremities. This often affects the feet during pregnancy but tends to occur in the later stages.
How Can I Keep My Feet Healthy During Pregnancy?
- Wearing orthotics can provide extra support for the feet and help distribute weight evenly
- Minimize the amount of time spent walking barefoot
- Wear shoes with good arch support
- Wear shoes that allow for good circulation to the feet
- Elevate feet if you experience swelling
- Massage your feet
- Get regular, light exercise, such as walking, to promote blood circulation to the feet
If you have any questions please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Are Bunions Affecting Your Everyday Life?
The Definition of Tarsal Tunnel Syndrome
Tarsal tunnel syndrome, though less commonly known than other foot conditions, can cause significant discomfort and impairment for those affected. Similar to carpal tunnel syndrome in the wrist, tarsal tunnel syndrome involves compression of the posterior tibial nerve as it passes through a narrow space in the ankle called the tarsal tunnel. This compression can result from various factors, including injury, inflammation, or underlying conditions like arthritis or diabetes. Symptoms of tarsal tunnel syndrome may include burning pain, tingling, numbness, or weakness in the foot and ankle, often worsened by prolonged standing or walking. Left untreated, tarsal tunnel syndrome can lead to permanent nerve damage and functional limitations. Diagnosis typically involves a thorough physical examination, along with imaging studies like MRI or nerve conduction tests. Early recognition and intervention are critical for managing tarsal tunnel syndrome effectively and minimizing long-term consequences. If you have any of the above symptoms, it is suggested that you confer with a podiatrist who can offer you effective treatment solutions.
Tarsal tunnel syndrome can be very uncomfortable to live with. If you are experiencing tarsal tunnel syndrome, contact Julie Jurd-Sadler, DPM of Progressive Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Tarsal Tunnel Syndrome
Tarsal tunnel syndrome, which can also be called tibial nerve dysfunction, is an uncommon condition of misfiring peripheral nerves in the foot. The tibial nerve is the peripheral nerve in the leg responsible for sensation and movement of the foot and calf muscles. In tarsal tunnel syndrome, the tibial nerve is damaged, causing problems with movement and feeling in the foot of the affected leg.
Common Cause of Tarsal Tunnel Syndrome
- Involves pressure or an injury, direct pressure on the tibial nerve for an extended period of time, sometimes caused by other body structures close by or near the knee.
- Diseases that damage nerves, including diabetes, may cause tarsal tunnel syndrome.
- At times, tarsal tunnel syndrome can appear without an obvious cause in some cases.
The Effects of Tarsal Tunnel Syndrome
- Different sensations, an afflicted person may experience pain, tingling, burning or other unusual sensations in the foot of the affected leg.
- The foot muscles, toes and ankle become weaker, and curling your toes or flexing your foot can become difficult.
- If condition worsens, infections and ulcers may develop on the foot that is experiencing the syndrome.
A physical exam of the leg can help identify the presence of tarsal tunnel syndrome. Medical tests, such as a nerve biopsy, are also used to diagnose the condition. Patients may receive physical therapy and prescriptive medication. In extreme cases, some may require surgery.
If you have any questions please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
The Necessity and Benefits of Hammertoe Surgery

Hammertoe, a deformity characterized by an abnormal bending of the toe joint, can lead to discomfort, difficulty walking, and even pain during daily activities. While many cases of hammertoe can be managed with conservative measures such as padding, shoe modifications, and orthotic devices, surgery may be necessary in certain instances. Hammertoe surgery becomes essential when the condition progresses to a point where conservative treatments no longer provide relief or when the deformity interferes significantly with mobility and quality of life. During surgery, the surgeon may release tight tendons, reposition bones, or remove damaged tissue to straighten and realign the affected toe. Although surgery involves risks like any medical procedure, it can offer long-term relief and improve functionality for individuals suffering from severe hammertoe deformities. If you are living with hammertoe, it is strongly suggested that you are under the care of a podiatrist who can determine if surgery is the correct choice for you.
Foot surgery is sometimes necessary to treat a foot ailment. To learn more, contact Julie Jurd-Sadler, DPM of Progressive Podiatry. Our doctor will assist you with all of your foot and ankle needs.
When Is Surgery Necessary?
Foot and ankle surgery is generally reserved for cases in which less invasive, conservative procedures have failed to alleviate the problem. Some of the cases in which surgery may be necessary include:
- Removing foot deformities like bunions and bone spurs
- Severe arthritis that has caused bone issues
- Cosmetic reconstruction
What Types of Surgery Are There?
The type of surgery you receive will depend on the nature of the problem you have. Some of the possible surgeries include:
- Bunionectomy for painful bunions
- Surgical fusion for realignment of bones
- Neuropathy decompression surgery to treat nerve damage
Benefits of Surgery
Although surgery is usually a last resort, it can provide more complete pain relief compared to non-surgical methods and may allow you to finally resume full activity.
Surgical techniques have also become increasingly sophisticated. Techniques like endoscopic surgery allow for smaller incisions and faster recovery times.
If you have any questions please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Causes and Symptoms of Cracked Heels
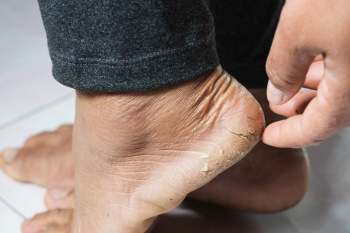
Cracked heels occur when the skin around the heels becomes dry, thickened, and fissured. This condition is often caused by a lack of moisture, leading to the skin's inability to retain hydration and elasticity. While anyone can develop cracked heels, some individuals are at a higher risk. Those who frequently expose their feet to harsh conditions, such as prolonged standing, walking barefoot, or wearing open-back shoes, are more susceptible. Additionally, factors like obesity, diabetes, and aging can contribute to the development of cracked heels. Symptoms of cracked heels include dryness, flakiness, redness, itching, and the formation of deep cracks or fissures. These fissures can be painful and may bleed in severe cases. It is essential to address cracked heels promptly to prevent complications such as infections. If you have developed cracked heels, it is strongly suggested that you consult a podiatrist who can provide the appropriate treatment methods.
Cracked heels are unsightly and can cause further damage to your shoes and feet. If you have any concerns, contact Julie Jurd-Sadler, DPM from Progressive Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Cracked Heels
Cracked heels appear unappealing and can make it harder for you walk around in sandals. Aside from looking unpleasant, cracked heels can also tear stockings, socks, and wear out your shoes. There are several methods to help restore a cracked heel and prevent further damage.
How Do You Get Them?
Dry skin is the number one culprit in creating cracked heels. Many athletes, walkers, joggers, and even swimmers suffer from cracked heels. Age and skin oil production play a role to getting cracked heels as well.
Promote Healing
Over the counter medicines can help, especially for those that need instant relief or who suffer from chronic dry feet.
Wear Socks – Wearing socks with medicated creams helps lock in moisture.
Moisturizers – Applying both day and night will help alleviate dryness which causes cracking.
Pumice Stones – These exfoliate and remove dead skin, which allows for smoother moisturizer application and better absorption into the skin.
Change in Diet
Eating healthy with a well-balanced diet will give the skin a fresh and radiant look. Your body responds to the kinds of food you ingest. Omega-3 fatty acids and zinc supplements can also revitalize skin tissue.
Most importantly, seek professional help if unsure how to proceed in treating cracked heels. A podiatrist will help you with any questions or information needed.
If you have any questions, please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Understanding the Symptoms of Cuboid Syndrome
Cuboid syndrome, a relatively uncommon but painful condition, occurs when the cuboid bone in the foot becomes displaced or irritated, leading to discomfort and limited mobility. The cuboid bone is located on the outer side of the foot, near the middle, and plays an important role in maintaining foot stability and movement. Diagnosis of cuboid syndrome involves a thorough physical examination by a podiatrist, focusing on the foot's range of motion, tenderness, and specific movements that reproduce pain. Imaging tests such as X-rays or MRI scans may be utilized to rule out other potential causes of foot pain and confirm the diagnosis. Symptoms of cuboid syndrome typically include pain on the outer side of the foot, difficulty walking or bearing weight, swelling, and a sensation of instability or shifting in the midfoot area. In severe cases, manipulation or mobilization techniques by a podiatrist may be necessary to realign the cuboid bone and alleviate symptoms. If you have pain in this part of your foot, it is suggested that you visit a podiatrist who can successfully diagnose and treat cuboid syndrome.
Cuboid syndrome, also known as cuboid subluxation, occurs when the joints and ligaments near the cuboid bone in the foot become torn. If you have cuboid syndrome, consult with Julie Jurd-Sadler, DPM from Progressive Podiatry. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Cuboid syndrome is a common cause of lateral foot pain, which is pain on the outside of the foot. The condition may happen suddenly due to an ankle sprain, or it may develop slowly overtime from repetitive tension through the bone and surrounding structures.
Causes
The most common causes of cuboid syndrome include:
- Injury – The most common cause of this ailment is an ankle sprain.
- Repetitive Strain – Tension placed through the peroneus longus muscle from repetitive activities such as jumping and running may cause excessive traction on the bone causing it to sublux.
- Altered Foot Biomechanics – Most people suffering from cuboid subluxation have flat feet.
Symptoms
A common symptom of cuboid syndrome is pain along the outside of the foot which can be felt in the ankle and toes. This pain may create walking difficulties and may cause those with the condition to walk with a limp.
Diagnosis
Diagnosis of cuboid syndrome is often difficult, and it is often misdiagnosed. X-rays, MRIs and CT scans often fail to properly show the cuboid subluxation. Although there isn’t a specific test used to diagnose cuboid syndrome, your podiatrist will usually check if pain is felt while pressing firmly on the cuboid bone of your foot.
Treatment
Just as the range of causes varies widely, so do treatments. Some more common treatments are ice therapy, rest, exercise, taping, and orthotics.
If you have any questions, please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Hammertoe and Its Causes
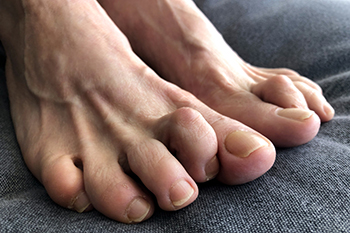
Hammertoe is a foot deformity characterized by an abnormal bending of the toe joints, causing the affected toe to resemble a hammer or claw. This condition typically affects the second, third, or fourth toes. It results from an imbalance in the muscles, tendons, and ligaments that control toe movement. Tightening of the ligaments and tendons, often due to wearing ill-fitting shoes with narrow toe boxes or high heels, can force the toes into a bent position over time. Additionally, genetic predisposition, foot structure abnormalities, and underlying conditions like arthritis or nerve damage can contribute to the development of hammertoes. As the condition progresses, individuals may experience pain, discomfort, corns, or calluses on the affected toes, making it difficult to wear shoes comfortably. Early intervention through proper footwear, toe exercises, orthotic devices, and, in severe cases, surgical correction can help alleviate symptoms and prevent complications associated with hammertoe. If you have hammertoe, it is suggested that you seek guidance from a podiatrist for an appropriate diagnosis and management of this condition.
Hammertoes can be a painful condition to live with. For more information, contact Julie Jurd-Sadler, DPM of Progressive Podiatry. Our doctor will answer any of your foot- and ankle-related questions.
Hammertoe
Hammertoe is a foot deformity that occurs due to an imbalance in the muscles, tendons, or ligaments that normally hold the toe straight. It can be caused by the type of shoes you wear, your foot structure, trauma, and certain disease processes.
Symptoms
- Painful and/or difficult toe movement
- Swelling
- Joint stiffness
- Calluses/Corns
- Physical deformity
Risk Factors
- Age – The risk of hammertoe increases with age
- Sex – Women are more likely to have hammertoe compared to men
- Toe Length – You are more likely to develop hammertoe if your second toe is longer than your big toe
- Certain Diseases – Arthritis and diabetes may make you more likely to develop hammertoe
Treatment
If you have hammertoe, you should change into a more comfortable shoe that provides enough room for your toes. Exercises such as picking up marbles may strengthen and stretch your toe muscles. Nevertheless, it is important to seek assistance from a podiatrist in order to determine the severity of your hammertoe and see which treatment option will work best for you.
If you have any questions, please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Heel Pain Can Be Treated!
More...
What Feet Can Reveal About Overall Health

Feet, often overlooked, hold valuable clues about our overall health and well-being. Various signs and symptoms manifesting in the feet can serve as indicators of underlying health conditions. For instance, changes in skin color or texture may signify circulatory issues or skin disorders, while brittle or discolored toenails can hint at fungal infections or nutritional deficiencies. Swelling in the feet and ankles may be from fluid retention, heart problems, or kidney issues. Furthermore, nerve damage in the feet can be an early sign of conditions like diabetes or neuropathy. Additionally, foot pain and discomfort can result from musculoskeletal problems, arthritis, or wearing improper footwear. Regularly inspecting and caring for our feet can help detect potential health concerns early and facilitate timely intervention. By paying attention to the signals our feet convey, we can take proactive steps to safeguard our well-being and maintain optimal health. If you are experiencing any foot pain or discomfort, it is strongly suggested that you visit a podiatrist who can help you with relief and treatment solutions.
When dealing with systemic disease of the feet, it is extremely important to check the affected areas routinely so that any additional problems are caught quickly. If you have any concerns about your feet and ankles contact Julie Jurd-Sadler, DPM from Progressive Podiatry. Our doctor will assist you with all of your podiatric needs.
Systemic Diseases of the Feet
Systemic diseases affect the whole body, and symptoms usually are displayed in the feet. This condition can make a patient’s ability to walk unbearable. Systemic diseases include gout, diabetes mellitus, neurological disorders, and arthritis.
Gout – is caused by an excess of uric acid in the body. Common symptoms include pain, inflammation, and redness at the metatarsal/phalangeal joint of the base big toe. Gout can be treated by NSAIDs to relieve pain and inflammation, and other drugs that lower the acid levels in the body.
Diabetes mellitus – is an increase in the level of blood sugar that the body cannot counteract with its own insulin. Failure to produce enough insulin is a factor in Diabetes.
Diabetes of the Feet
Diabetic Neuropathy – may lead to damaged nerves and affect the feet through numbness and loss of sensation.
Peripheral Vascular Disease – can restrict the blood flow to the feet, and often times lead to amputation of the feet.
If you have any questions please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Pain Caused by Working on Your Feet

If you are experiencing foot pain after a long day on your feet at work, you are not alone. The fatigue from standing all day can lead to discomfort, but if the foot pain persists, it may indicate more serious issues such as plantar fasciitis or heel spurs. Several factors contribute to foot pain and fatigue after working, including having inadequate support in your shoes, particularly if you are on hard surfaces like concrete or tile. Uneven pressure distribution within the foot and poor circulation can make the problem worse, leading to swelling and further discomfort. Additionally, existing foot conditions like bunions and Morton’s neuroma can intensify the pain. To alleviate foot pain after work, consider investing in supportive footwear with cushioned soles, taking breaks to stretch and walk, and wearing compression socks if circulation is an issue. Incorporating foot exercises and stretches into your daily routine can also help improve foot strength and flexibility, reducing the likelihood of pain. If foot pain persists, it is suggested that you schedule an appointment with a podiatrist for proper diagnosis and treatment options.
While working on the feet, it is important to take the proper care of them. For more information about working on your feet, contact Julie Jurd-Sadler, DPM from Progressive Podiatry. Our doctor will treat your foot and ankle needs.
Working on Your Feet
Standing on your feet for long periods of time can cause stress and pain in your feet. Your whole body may experience change in terms of posture, back pain, bunions, callouses and or plantar warts. There are ways to avoid these conditions with proper foot care, smart choices and correct posture.
Positive Changes
Negative heeled shoe – Choosing this shoe type places the heel slightly lower than the ball of the foot. These are great for overall foot health. Find shoes that fit you correctly.
Go barefoot – Our feet were not designed to be enclosed for all hours of the day. Try to periodically expose your feet to air.
Eliminate Pain
Foot Exercises – Performing simple exercises, incorporating yoga and doing stretches are beneficial. This will allow increased blood flow to the area and muscles of the foot.
Achilles tendon – Stretching the foot out flat on the floor will relax the calf muscles and tendon. These exercises can be performed almost anywhere. Make sure you add these exercises to your daily regimen.
With a little bit of this information and knowing more about foot health, you will notice changes. Foot stretches and proper footwear will help with pain and prevent further issues.
If you have any questions please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Possible Foot Problems From Wearing High Heels

High heels, while fashionable, can lead to various foot problems due to their design and the way they alter the natural mechanics of walking. One common issue is the development of bunions, where the pressure and narrow toe box of high heels force the big toe to bend outward, causing a painful bony bump to form. Additionally, wearing high heels regularly can shorten the Achilles tendon and calf muscles, leading to stiffness and discomfort when walking in flat shoes. High heels also increase pressure on the ball of the foot, potentially causing metatarsalgia, a painful condition characterized by inflammation and discomfort in the ball of the foot. Furthermore, the instability caused by high heels can contribute to ankle sprains and instability over time. To mitigate these issues, it is important to limit high heel wear, opt for lower, wider heels when possible, and incorporate foot-strengthening exercises into your routine to counteract the negative effects of high heels on foot health. If you wear high heels and have developed specific foot conditions, it is suggested that you consult a podiatrist who can effectively treat any foot ailment that has arisen, and offer other footwear choices.
High heels have a history of causing foot and ankle problems. If you have any concerns about your feet or ankles, contact Julie Jurd-Sadler, DPM from Progressive Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Effects of High Heels on the Feet
High heels are popular shoes among women because of their many styles and societal appeal. Despite this, high heels can still cause many health problems if worn too frequently.
Which Parts of My Body Will Be Affected by High Heels?
- Ankle Joints
- Achilles Tendon – May shorten and stiffen with prolonged wear
- Balls of the Feet
- Knees – Heels cause the knees to bend constantly, creating stress on them
- Back – They decrease the spine’s ability to absorb shock, which may lead to back pain. The vertebrae of the lower back may compress.
What Kinds of Foot Problems Can Develop from Wearing High Heels?
- Corns
- Calluses
- Hammertoe
- Bunions
- Morton’s Neuroma
- Plantar Fasciitis
How Can I Still Wear High Heels and Maintain Foot Health?
If you want to wear high heeled shoes, make sure that you are not wearing them every day, as this will help prevent long term physical problems. Try wearing thicker heels as opposed to stilettos to distribute weight more evenly across the feet. Always make sure you are wearing the proper shoes for the right occasion, such as sneakers for exercising. If you walk to work, try carrying your heels with you and changing into them once you arrive at work. Adding inserts to your heels can help cushion your feet and absorb shock. Full foot inserts or metatarsal pads are available.
If you have any questions please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
What Causes Cracked Heels?
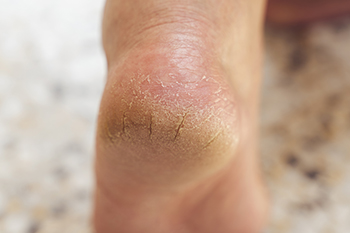
Cracked heels, a common foot ailment, can be traced back to various factors that contribute to their unsightly appearance and discomfort. Inadequate moisturization emerges as a primary culprit, as neglecting to keep the skin hydrated can lead to dryness and fissures. Prolonged standing or walking on hard surfaces exerts excessive pressure on the heels, causing them to crack. Wearing ill-fitting shoes exacerbates the issue, rubbing against the skin and creating friction that weakens the natural barrier. Additionally, exposure to harsh weather conditions, such as extreme heat or cold, can strip the skin of its moisture, making it prone to cracking. Poor foot hygiene and improper foot care practices may further contribute to the development of cracked heels. Cracked heels can be painful, and if you have developed this condition, it is suggested that you confer with a podiatrist who can prescribe medication for effective relief.
If the skin on your feet starts to crack, you may want to see a podiatrist to find treatment. If you have any concerns, contact Julie Jurd-Sadler, DPM from Progressive Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Cracked Heels
It is important to moisturize your cracked heels in order to prevent pain, bleeding, and infection. The reason cracked heels form is because the skin on the foot is too dry to support the immense pressure placed on them. When the foot expands, the dry skin on the foot begins to split.
Ways to Help Heal Them
- Invest in a good foot cream
- Try Using Petroleum Jelly
- Ease up on Soaps
- Drink Plenty of Water
Ways to Prevent Cracked Heels
- Moisturize After Showering
- Skip a Shower
- Keep Shower Water Lukewarm
- Don’t Scrub Your Feet
If you are unsure how to proceed in treating cracked heels, seek guidance from a podiatrist. Your doctor will help you with any questions or information you may need.
If you have any questions, please feel free to contact our offices located in Ijamsville and Mouth Airy, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Blog Archives
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019